By Aneri Pattani & Rebecca Moss| Spotlight PA
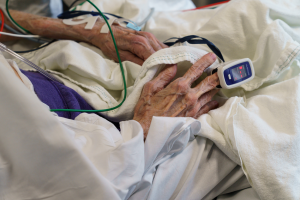
Pennsylvania’s plan to protect its nursing homes was robust and aggressive.
In mid-March, before the coronavirus had widely taken hold across the state, emergency response officials drafted a three-page blueprint for quick strike teams of medical professionals that would respond to facilities as soon as a few positive cases were confirmed.
The teams — made of epidemiologists, nurses, emergency management personnel, and medical experts — would show up at a facility within six hours of a call for help, according to internal documents obtained by LevittownNow.com news partners Spotlight PA. Within two hours, they would complete an assessment of the facility’s needs and create a plan to address them.
The teams would train nursing home staff on infection prevention protocols, provide personal protective equipment, help identify secluded quarantine areas, gather information for visitor and staff contact tracing, confirm a staffing plan, and more, according to the documents.
The quick response plan was circulated within the health department, with emails showing staff nurses and others were asked to volunteer. In the third week of March, it was shared with providers, said Zachary Shamberg, president and CEO of the Pennsylvania Health Care Association, which represents more than 400 long-term care facilities.
But the plan was never fully implemented, and a similar — though far more limited — effort wasn’t activated until mid-April, long after major outbreaks had already taken hold.
“This was being touted as the answer to the epidemic,” Shamberg said. “This was the state support we were counting on.”
“I have to believe if these teams had been ready and prepared, we’d be in a much better place than we are today.”
A spokesperson for the state health department, April Hutcheson, said she was unaware of the quick response team plan, but noted that many of the concepts that were part of it have been implemented. The state has been trying to provide as much help as possible “virtually,” she said.
State Health Secretary Rachel Levine said nursing homes have always been a priority.
“I don’t think our initial and our continuing plans have been misguided at all,” Levine said at a Monday news conference. “We have been working very hard throughout this entire process on protecting those homes as much as possible. It’s a significant challenge, and we’re continuing to do the very best we can.”
The outbreak of COVID-19 was always feared to be particularly acute among older populations in Pennsylvania, which has one of the highest numbers of nursing homes in the U.S. But a growing chorus of providers, advocates, lawmakers, families, and residents now say that state officials were too slow to act and are still not doing enough to help.
In the meantime, some facilities have become death traps.
As of Wednesday, Bucks County reported that 82 percent of all COVID-19 patient deaths within its borders have been residents of long-term care facilities. More than half of the licensed centers in the county have at least one COVID-19 case, with sources stating several have more than a dozen cases. Data has shown that the majority of new cases in recent weeks have been of residents and staff at those centers.
As of Friday, state officials reported infections at 522 facilities and 2,458 deaths statewide, which is 68 percent of all COVID-19 fatalities statewide. Roughly 900 new deaths in these facilities have been reported in just the past week. Despite the alarming numbers, the administration has stuck by its modest goals for increased statewide testing and has not committed to wider testing at nursing homes.
By contrast, Maryland, West Virginia, Wisconsin, Massachusetts, and Tennessee have committed to testing all long-term care residents and staff. In Maryland and Massachusetts, health officials also have formed “strike teams” to help overwhelmed facilities navigate outbreaks and mitigate the spread.
Levine said at a legislative hearing Thursday that state officials were discussing strategies to expand testing. But Sen. Lisa Baker (R., Luzerne) countered, “The time for robust discussing is over and the time for action is now.”
The first positive cases of COVID-19 at the Life Care Center in Washington state were announced on February 28 — a full week before any coronavirus cases were identified in Pennsylvania, and several weeks before news outlets first reported cases in nursing homes here.
As soon as that news broke, Pennsylvania officials should have visited facilities, prioritizing those with a history of infection control issues, to assess if they had enough staff and protective equipment, said Diane Menio, executive director of the Center for Advocacy for the Rights & Interests of the Elderly.
“Not just looking at data, but going in and making sure there were people there and that they had a plan,” Menio said. “But that wasn’t happening.”
State health officials said they began sending advisories about COVID-19 to nursing homes in January. Since then, Hutcheson said, the department has provided guidance on separating sick staff and residents from those who are healthy, offered consultations on infection control, and regularly sent facilities personal protective equipment — even as lawmakers, families, and facility staff said supplies remain scarce.
Although the department doesn’t have quick response teams by that name, Hutchseon said, “in effect, those things are happening.”
“Any provider who wants support and consultation is getting that support and consultation,” she said, adding that the National Guard has been used to assist on the ground.
In early April, the Pennsylvania National Guard sent medics and nurses to a few facilities where a significant number of staff were out sick, spokesperson Lt. Col. Keith Hickox said. As the requests for support increased, the guard on April 22 began dispatching a crew to distressed facilities to assess their needs — similar to the original strike team plans.
To date, the guard has visited just 11 facilities — 2 percent of those reporting cases — and along with supporting testing sites around the state, the guard’s medical assets are now near capacity, Hickox said.

Credit: Charles Fox/Philadelphia Inquirer
‘I’ve never seen this in my life’
It’s hard to assess the effectiveness of the state’s response or which nursing homes are facing the biggest crises because the Wolf administration has refused to release a facility-by-facility list, even as neighboring states — including New York, New Jersey, Maryland, and Ohio — have done so.
Bucks County officials have also declined to release information on facilities with cases aside from the county-run Neshaminy Manor.
Federal regulators are taking steps to make facility data public, but it’s unclear when it will be available. Advocacy groups, including the AARP of Pennsylvania, have called on Wolf to reverse course, saying that information is critical to accountability.
Numerous families statewide and in Bucks County are only learning about cases from the news or after their mothers, fathers, or siblings have already tested positive for the virus or died from it. And there are also concerns about how well providers are protecting their residents and staff.
Federal regulators have halted regular inspections, and the state has said it would only investigate complaints that indicate patients are in immediate jeopardy. What’s more, state health officials are refusing to say if they have conducted inspections or issued violations at any particular facility in relation to COVID-19, saying the public must wait until they post information online.
That typically takes more than a month, and could be delayed even longer because of the outbreak.
Facilities have banned visitors in most cases, and in-person ombudsman programs — advocates, often volunteers, that act as the voice for at-risk patients — have been communicating only by intermittent video or phone calls since mid-March. Taken together, facilities — including those with bad track records — have been left to largely police themselves.
“It’s not enough for the facility to say what they think their needs are,” said Lori Smetanka, executive director of the National Consumer Voice for Quality Long-Term Care. “There really needs to be some outside assessors that also have different areas of expertise to go in and assess what’s really happening.”
Devastating stories are emerging from across the state.
Nurses at the Gardens at West Shore in Cumberland County told Spotlight PA they are testing positive for the coronavirus and being told to “take Tylenol and come back.” They were instructed not to test residents with symptoms of the virus, they said, and were forbidden from telling families and other residents about cases. Sick residents that had been moved to a separate area were later moved back among the general population. And nurses said they are reusing each other’s protective gear, and often wear the same gowns between caring for well and sick residents.
“Multiple people have reported this to the Pennsylvania Department of Health and nothing has been done,” said one nurse, who requested anonymity because she was not allowed to speak with the media. “These people are sick. They need more help than they are given.”
The facility is one of four in Pennsylvania and 88 nationwide flagged by federal regulators because of a long record of persistent and serious care issues. It is also among 27 facilities in the country that have failed to improve despite that designation, according to a recent report by the Centers for Medicare and Medicaid Services.
“I’ve never seen this in my life, in my 30 years of nursing,” said one nurse at Gardens at West Shore, who is recovering from the coronavirus at home and asked not to be named for fear of retaliation. “Everybody was scared. … Our residents didn’t know what was going on. We couldn’t really tell them. People are crying because they don’t want to lose their job.”
A spokesperson for the state health department, Nate Wardle, declined to say if any assistance had been provided to the facility.
Beverly Fry, the administrator at Gardens at West Shore, said nurses were only returning to work after being allowed by a medical professional. When asked about whether the facility had instructed nurses not to test residents, she said, “Oh my,” and referred the news organization to a statement that said the facility has followed all state and federal guidelines.
The owner of the home, Priority Healthcare Group, did not respond to a request for comment.
At least 71 people have died at the Brighton Rehabilitation and Wellness Center in Beaver County, where weeks ago facility administrators said they presumed the more than 750 residents and staff all had the virus. The state quietly appointed a temporary management company to run the center in mid-April, and lawmakers in the region have called for a federal investigation into the nursing home. Brighton is one of 16 state facilities listed as a candidate for additional federal oversight because of documented problems.
And as of Wednesday, 34 people had died at the Southeastern Veterans’ Center in Chester County. The death toll there nearly tripled over a five-day stretch in April, but the home concealed the extent of the outbreak from families and the public, according to internal documents obtained by The Philadelphia Inquirer.

Credit: Dan Gleiter/PennLive
Limited help for overwhelmed facilities
Absent more of a presence on the ground, the state has relied on a nearly $1 million contract with ECRI, a patient safety and health-care research institute headquartered in Plymouth Meeting. The company was hired to consult with nursing homes on proper infection prevention methods, and as questions about the state’s response have increased, Levine, the health secretary, has repeatedly touted ECRI’s work, but provided few details.
“They can even do sort of a virtual walk around the facility to make sure that everything is being done to protect the staff as well as patients,” Levine said on April 6.
But in an interview with Spotlight PA, ECRI management said it was only conducting phone consultations, and that the company had offered to send iPhones to facilities to do video consultations, but was told the health department preferred phone calls.
ECRI has a team of six nurses trained in infection control who consult with any facilities referred to them by the health department. The nurses correct improper protocols that might spread the virus, and then follow up with the facility for several weeks to see if practices improve. They also help facilities request personal protective equipment from the health department.
“Some facilities are so overwhelmed that people don’t pick up the phone,” said Karen Schoelles, ECRI’s vice president of clinical excellence and safety, and head of the team working for the state. At others, staff answer the phone in tears, traumatized from seeing coworkers get sick and patients die daily.
As of April 29, ECRI had consulted with 76 facilities, or about 15 percent of all long-term care facilities with cases reported to the state. Providers criticized that number as too low when hundreds of facilities are vying for support.
“If ECRI is the be-all, end-all of the state’s response at this point, why have they not been to every facility?” Shamberg said.
Schoelles said ECRI can only work with facilities referred by the state. It receives three to six referrals a day, she said, but could handle up to 10. Hutcheson, the health department spokesperson, said the state’s healthcare-associated infection staff is taking the lead on phone consultations and ECRI is supplementing their efforts.
“We utilize ECRI quite frequently when we need to,” she said.
The state’s long-term care ombudsman, Margaret Barajas, said her office is currently taking resident complaints by phone and is hoping to create a virtual visiting service soon to see the conditions inside facilities. But without widespread testing and protective gear at nursing homes, she fears the number of deaths will continue rising.
“We may have flattened the curve,” Barajas said, “but I don’t believe the consumers I am responsible for advocating on behalf are any safer today than they were in early March.”
To report concerns about a long-term care facility, you can contact the state ombudsman’s office at (717) 783-8975.
PennLive staff reporter Charles Thompson contributed to this article.
Spotlight PA is an independent, nonpartisan newsroom powered by The Philadelphia Inquirer in partnership with the Pittsburgh Post-Gazette and PennLive/Patriot-News. Sign up for our free weekly newsletter.
Spotlight PA receives funding from nonprofit institutions and readers like you who are committed to investigative journalism that gets results. Give a gift today at spotlightpa.org/donate.








